Do you remember the days you would visit an entertainment joint with friends and feel out of place because you don’t take alcohol?
The first thing they’ll tell you is how good the drink, popularly known as ‘kamnyweso’, feels, and that you need to take a sip. After a few weeks, you graduate to a bottle then two, and the story goes on. Finally, you can’t do without it.
The happy feeling that comes after taking alcohol could be what drives you. However, experts say that with time, your essential organs, including the liver, pay the price.
Peter Kariuki, 30, narrates how scared he was when he was told that his liver was damaged due to excessive alcohol intake.
He began taking alcohol in 2005 while in high school due to peer pressure. “I started taking beer then changed to chang’aa,” he says.
Peter says in 2024, after taking alcohol for nine years, the effects were evident since he started feeling body itchiness he couldn’t explain. The doctor’s report then stated that he had fatty liver disease, a condition where fats are deposited in the liver, and that he should stop taking alcohol.
However, this was difficult for Peter for he tried for only a few weeks and went back to his trend. “I was taken for rehab but after some time, I relapsed,” he says.
He says it was easy for him to access chang’aa because of the proximity and affordability, making it easy for him to relapse.
The situation worsened in 2025, when his stomach started swelling, his skin and eyes turned yellow and he started vomiting blood.
“I thought sasa nitadead because they told me that my liver imedead (I thought I would die because they told me my liver had died),” he says. “I was worried.”
Kariuki, who is a civil servant, says he has stopped taking alcohol and every time he thinks about the consequences and how his young family will suffer, he vows never to taste the drink again.
“I only visit the club to buy alcohol for my friends,” he says jokingly.
AVOIDING DISASTER
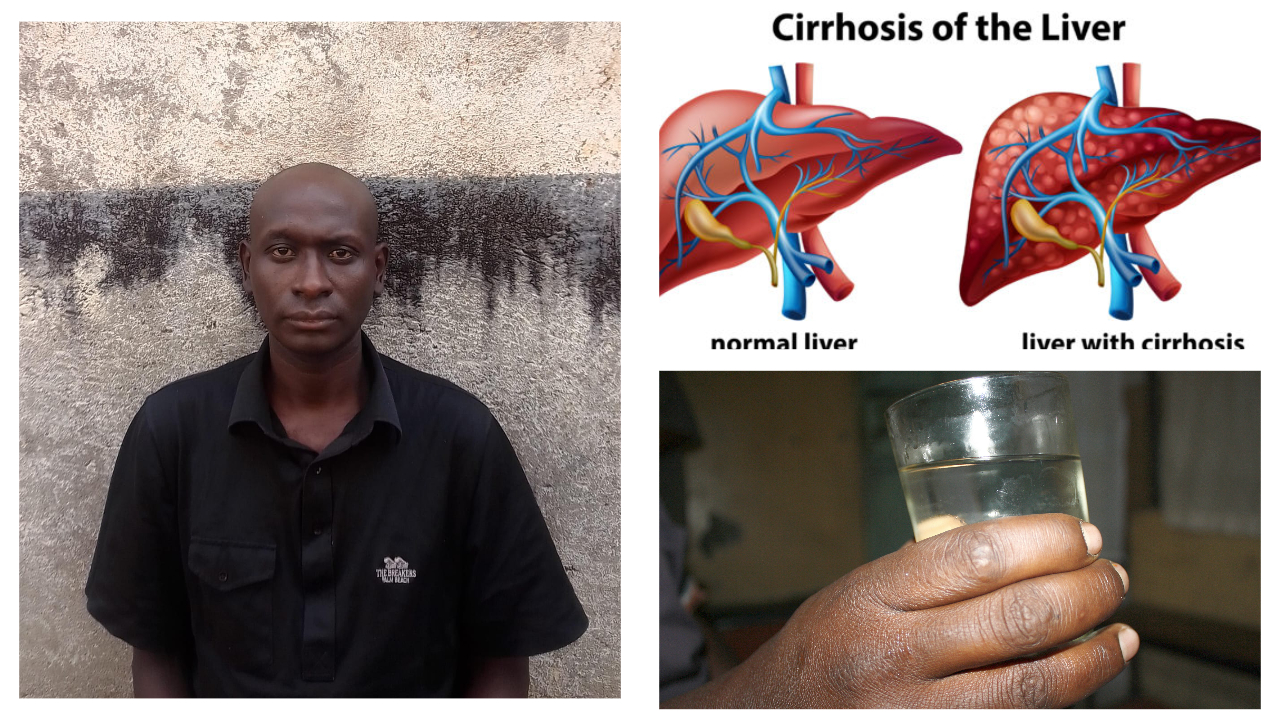
Dr Maureen Kaunda, a liver expert from the Ministry of Health’s Noncommunicable Diseases division, consistent excessive intake of alcohol for 10 years causes alcoholic liver cirrhosis, which is the permanent scarring of the liver.
The liver is the centre where alcohol is metabolised, she explains.
In the initial stages, one develops fatty liver disease every time he or she drinks heavily. It then graduates to alcoholic hepatitis, which is the inflammation of the liver and can come after three to five years of consistently taking excessive alcohol. Eventually it progresses to alcoholic liver cirrhosis.
She says it is possible for one to avoid damaging the liver if you stop taking alcohol at the first stage of fatty liver disease.
“The condition is reversible at this stage if someone stops drinking alcohol since the liver forgives easily and regenerates itself with time,” Kaunda says.
She says the liver also gets tired of performing its function of detoxifying your body as you continue taking alcohol. The liver stops its other functions any time you take alcohol to remove the alcohol from the body first but can get overwhelmed.
She warns that if the condition progresses to alcoholic liver cirrhosis, it is only possible to treat the symptoms, which include yellowing of the eyes and skin, abdominal pains, swollen legs, vomiting blood and, in its last stage, confusion. The jaundice by-product could progress to the brain, she warns.
Once the liver is damaged due to liver cirrhosis, there is no drug that can restore it. However, further damage stops if the patient stops taking alcohol.“One would argue that since it is only a bottle a day, I will be okay,” Kaunda says.
“But the likelihood of increasing your alcohol intake once you start is high. Therefore, it is advisable that you abstain from alcohol intake.”
DIGESTION MYTH
Nutritionist Erec Ngeso debunks the narrative that a glass of alcohol after a meal helps in digestion.
He says although men can digest more alcohol than women (two bottles to one), excessive intake can cause undernutrition.
Once addicted, one focuses more on the intake of alcohol than food.
You are considered a heavy drinker if you take four bottles of alcohol a day or 14 and above bottles of alcohol a week.
The cost of treating liver cirrhosis is still a challenge for those with no medical cover. Kaunda says although SHA can cover treatment for the symptoms or when one is admitted, rehabilitation cost is an individual’s responsibility.
She adds that liver transplant is the ultimate cure for alcoholic liver cirrhosis. However, Kenya is yet to make such medical advancements. “We only give supportive management for this condition,” the liver expert says.
Most patients are advised to stop alcohol intake as the best step towards recovery. This is not easy, however. Counsellor James Kariuki says it requires one to be in a controlled environment, such as a rehabilitation centre. It will be possible to ensure accountability in such set-ups, he says.
“One has to be determined and willing to quit,” he says.
“Otherwise, they can go back to alcohol use even after the end of the rehab programme.”
BINGE DRINKING CRISIS
Data indicates that up to 18,458 people in Kenya are living with liver cirrhosis due to alcohol use, with 938 dying annually due to liver cirrhosis caused by alcohol use.
Nacada’s data on alcohol abuse in the year 2024 and 2025 shows that one in eight Kenyans, equivalent to 3.1 million, are users of alcohol.
Binge drinking stands at 12.7 to 13 per cent of the population. Men are the most affected at 19 per cent, with females at 6.8 per cent. In terms of regions, Western Kenya is leading at 23.8 per cent, followed by Coast and Central region.
In regards to alcohol-related liver cancer, a Lancet study in 2024 and 2025 shows that six out of 10 per cent of liver cancers in Kenya can be prevented by reducing alcohol consumption and treating hepatitis.
Kaunda says the Health ministry has been working towards ensuring that legislation on controlling alcohol abuse is enforced by making sure alcohol joints operate within the stated time.
Other measures include advocating for early identification of the disease and routine screening for harmful alcohol use.
“You can do self-examination to determine if you are doing badly and therefore need help,” she says.
by Charity Chigulu